
Prevention-The Key to Treating OSA/SDB-
Part II
Many morphometric features that
put adults at risk for OSA/SDB are present during childhood and
it is important for sleep specialists to recognize these features
and treat them early.
By Brian G. Palmer, DDS
Most lactation (breast-feeding) specialists know very little about
obstructive sleep apnea (OSA)/sleep-disordered breathing (SDB),
and most sleep specialists know very little about the importance
of breast-feeding. It is in the hopes that the second part of
this article will help educate both sides to the fact that there
is a strong relationship between the specialties, and that both
specialties will start working together to help study and prevent
the very serious medical condition called OSA/SDB.
There are no ideal treatments for OSA/SDB—all have potential
side effects. A tracheostomy, although usually 100% successful,
is not a choice most people would prefer. Patients who use continuous
positive airway pressure (CPAP) often have problems with compliance.
Surgeries do not always solve the challenges of OSA/SDB, and may
even make the condition worse. Oral appliances can move teeth
and cause malocclusions or create temporomandibular jaw (TMJ)
problems.
Christian Guilleminault, MD, cofounder of the Stanford University
Sleep Disorders Center, Stanford, Calif, stated at the 2002 American
Dental Sleep Medicine Conference in Seattle that prevention is
the best form of treatment for OSA/SDB. This author also believes
prevention is the key. In order to prevent OSA/SDB, however, one
needs to understand some of the factors that affect it. It is
important to note that OSA/SDB is not just limited to obese people
and there is more to OSA/SDB than the results from a sleep study.
Guilleminault has coauthored articles1-2 that describe
the risk factors of OSA. These factors include a high palate,
narrow dental arches, overjet, high body mass index (BMI), and
a large neck. If an individual does not have a high BMI or large
neck size, then the predictive factors for OSA are a high palate,
narrow dental arches, and overjet.
In another article by Guilleminault,3 he states that
inherited craniofacial features can be a strong indicator of risk
for developing OSA. Genes are factors in facial form; however,
many facial forms are influenced by habits.
Kushida et al4 stated that abnormal tongue activity
is also a predisposing factor for OSA. Some abnormal tongue activity
is genetically linked, but is mainly the result of bottle-feeding
and excessive noxious habits such as pacifier use, digit sucking,
lip sucking, arm sucking, and blanket sucking.5
Morphometric features
Anything that contributes to the blockage or collapse of the oral
cavity and/or airway space can contribute to OSA/SDB. Factors
that can contribute to blockage or collapse include:
* grossly enlarged tonsils and adenoids
* macroglossia
* elongated soft palates and enlarged uvulas
* polyps, tumors, and other abnormal growths
* facial-skeletal growth abnormalities
* central nervous system dysfunction affecting facial muscles
* ankyloglossia (tongue-tie)6
* large tori
* improper feeding of infants (using artificial bottles and nipples)
* noxious habits that include pacifier use, arm sucking, lip sucking,
blanket sucking, and excessive digit sucking
* drugs or diet7
Breast-feeding
Breast-feeding is important for the proper development of the
swallowing action of the tongue, shaping of dental arches, and
proper alignment of the teeth.8,9
The tongue contributes to the developmental shaping of the palate9
during its motion across the palate during a swallow. Insert a
bottle or pacifier between the tongue and the palate and the tongue
cannot reach the palate. The physical contact of the bottle-nipple/pacifier
can actually elevate the height of the palate. A vacuum created
by strong sucking actions during excessive noxious habits can
also increase the height of the palate.9
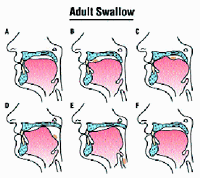 Figure
1. Adult swallowing pattern.
Figure
1. Adult swallowing pattern.
From a dental or oral cavity developmental perspective, the importance
of breast-feeding is for a proper swallowing pattern to be developed.
The swallowing pattern developed during infancy extends into adulthood.
A proper adult swallowing pattern (Figure 1) is initiated with
the tip of the tongue on the maxillary anterior papilla area just
behind the maxillary front teeth. The tongue then continues across
the hard palate in a peristaltic-like motion pushing either a
bolus of food or saliva ahead of the motion. Near the end of the
swallow, the tensor palatini muscles fire and open the eustachian
tubes. The levator palatini muscles and the tensor palatini muscles
elevate and tense the soft palate so that food and water will
not escape through the nose. During a normal correct swallow,
the tongue should not exert any pressure on any teeth. The tongue
should then rest against the anterior portion of the hard palate
until the next swallow.
During bottle feeding, a proper swallowing action may not develop
and a tongue-thrust may develop instead. Not much muscle coordination
is needed during most bottle-feeding, so perioral, facial, and
TMJ musculature may not develop properly. Some of the time during
bottle-feeding, the infant only needs to squeeze on the nipple
to express formula from the bottle. At other times, the infant
may have to suck excessively to remove formula from the bottle.
Since the hole at the tip of the nipple is not regulated to a
standard size, the size of the hole can be quite variable. A nipple
with a large hole may gush out an excessive amount of formula
that could possibly choke the infant. The infant has to place
the tongue at the back of the throat in a protective posture so
that too much formula does not go down the throat. If the hole
is too small, the infant may have to suck on the nipple excessively
to express the formula. As formula is removed, a vacuum can be
created inside the bottle. More suction is then needed to remove
the formula. The greater the sucking action needed within the
mouth, the greater the potential for collapse of the oral cavity.
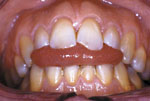 Figure
2. Adult tongue-thrust.
Figure
2. Adult tongue-thrust.
During bottle-feeding, the position and action of the tongue are
different than during breast-feeding. Since most bottle-nipples
are firmer than the breast, the tongue gets drawn inside the mouth
to protect the bottom side of the tongue from being traumatized
by the gum pad.10 A tongue-thrust (Figure 2, page 55)
is most likely to develop when this occurs. The excessive vacuum
that may be needed during bottle-feeding and the development of
a tongue-thrust are the main contributing factors to the malocclusions
that put an individual at risk for OSA/SDB. The above is also
true for excessive use of pacifiers, digit sucking, blanket sucking,
and arm sucking.5
Related articles
Paunio et al11 found that dummy and digit sucking was
strongly associated with malocclusion and found that 35% of 3-year-olds
had a malocclusion. Melsen et al12 found that digit
and dummy sucking resulted in increased tendency to tongue-thrust,
and tongue-thrusts were related to open bites, cross bites, overjet,
and Class II malocclusion. It was concluded that sucking habits
influence the etiology of malocclusion. Davis and Bell13
demonstrated that there was a strong association (P=>.0006)
between exclusive bottle-feeding and malocclusion, and that the
relationship did not diminish as the child grew from the primary
to permanent dentition.
A study by Farsi et al14 demonstrated that digit and
dummy sucking was the lowest among children who had a good opportunity
for breast-feeding and that there was a significant relationship
between sucking habits and malocclusion such as Class II malocclusion,
increased overjet, and anterior open bites. The principal finding
in the study by Labbok and Hendershot15 was that the
longer the duration of breast-feeding, the lower the incidence
of malocclusion. The study also found that bottle-feeding leads
to a habit of tongue-thrusting, and there was a significant decrease
in tongue-thrusting with an increased duration of breast-feeding.
A tongue-thrust is probably the biggest contributor to the development
of a malocclusion and to the relapse (failure) of most orthodontic
cases. To observe a tongue-thrust, one just has to have a person
with a malocclusion close the mouth, then slightly separate the
lips, and then have the individual swallow. If the individual
has a malocclusion with spaces anywhere in the mouth, one will
be able to see the tongue extend into the space(s) during the
swallow. Saliva may also ooze between the teeth. During a correct
swallow, the tongue should be on the roof of the mouth and the
saliva should be forced distally into the throat, not forward
between the teeth.
Adults do not form the morphometric characteristics that put them
at risk for OSA/SDB overnight. They had those characteristics
when they were young, but nobody understood or appreciated the
consequences of those characteristics.
In 1996, the American Academy of Pediatric Dentistry (AAPD)16
stated that 89% of youth, ages 12 to 17, had some occlusal disharmony,
and that 16% of youth had such severe handicapping malocclusion
that treatment was mandatory. In 1997, Victora et al17
conducted an epidemiological study, which showed that pacifiers
were commonly used by 85% of infants in her study by 1 month of
age. She also found that children weaned from breast-feeding early
use a pacifier more often than those who were breast-fed longer.
The Victora and AAPD findings should be alarming. Is it just by
chance that these percentages are so similar? This is extremely
significant once one realizes that in prehistoric times, and in
nonindustrialized cultures as recently as the 1930s,7 people had
minimal malocclusions.
Shepard et al18 stated that the largest increment of
craniofacial development occurs within the first 4 years of life
and that 90% of craniofacial development is complete by the age
of 12. Since 90% of craniofacial development has occurred by that
age, then it is very likely that the morphometric features that
put adults at risk for OSA/SDB were probably present at age 12.
Addressing and correcting these features early may significantly
reduce the medical problems that many children have as a result
of undiagnosed OSA or upper airway resistance syndrome. The most
important thing in life is one’s ability to breathe. A person’s
health is directly related to their ability to breathe oxygen.
If a child or an adult cannot breathe well, then their health
will be affected in some way.
Most children are not screened or tested for OSA/SDB and therefore
are not diagnosed with the condition. The reason for this is that
many physicians, especially pediatricians, are still unaware of
the relatively new field of OSA/SDB. Conditions such as bed wetting,19,20
behavioral problems,21 and attention deficit hyperactivity
disorder22 could possibly be prevented if infant sleep
problems were addressed early.
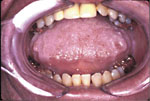
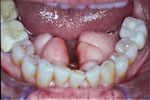
Figure 3. Massive tongue.
Figure 4. Adult
tori.
Oral Characteristics of Sleep Apnea
Anything that decreases the normal volume of the oral or nasal
cavity can contribute to OSA/SDB. Some factors that can contribute
to decreased size include tumors, large tongues, and tori. Large
tongues are due to genetics, while tori are due to clenching and
bruxing (Figures 3 and 4, page 56). Tongue-based obstructions
can be checked by pulling the tongue forward out of the mouth
with gauze and then having the person breathe while the tongue
is advanced. Those with obstructions at the tongue base can many
times immediately note better airflow. Obstructions to nasal airflow
can be checked by visual inspection using a nasal spectrum or
by blocking one side of the nose while having the patient breathe
through the other side. One should also note the shape and collapsibility
of the nose.23
Individuals with long face syndrome (LFS)24 are also
at high risk for having OSA/SDB. Although some individuals with
LFS have a genetic predisposition for it, many have the disorder
because of large tonsils or an obstruction in the airway that
forced them to become mouth breathers when they were youngsters.
The chronic mouth breathing can then lead to a narrowing or collapse
of the face.25
Conclusion
We are seeing just the tip of the iceberg when it comes to the
medical expenses associated with OSA/SDB. Most of the morphometric
features that put an adult at risk for OSA/SDB are present during
early childhood. It is up to health care providers to recognize
these features and treat them early. Many of our children are
suffering disorders related to airway resistance and poor quality
of sleep. By treating early, we, as a society, can have healthier
children as well as lowered health care costs. Treatments can
be as simple as rapid palatal expansion before the fusion of the
midpalatal suture line, removal of massive tonsils, or correction
of a Class II malocclusion at the proper growth period. Prevention
is the best and cheapest way to treat OSA/SDB. The best prevention
is breast-feeding and keeping pacifiers out of the mouths of our
children. Breast-feeding is the best form of health care we can
give children. It is free to all children. Not only are there
nutritional, immunological, and psychological benefits of breast-feeding,
there are also the benefits of a better occlusion and a reduced
risk of OSA/SDB. All health care providers need to understand
the benefits of breast-feeding and need to encourage it as much
as possible.
Brian G. Palmer, DDS, is a full-time general dentist in Kansas
City, Mo, who has a special interest in the cause, prevention,
and treatment of obstructive sleep apnea.
References
1. Kushida CA, Efron B, Guilleminault C. A predictive morphometric
model for the obstructive sleep apnea syndrome. Ann Intern Med.
1997;127(8 Pt 1):581-587.
2. Kushida CA, Guilleminault C, Ahmed O, Clerk AA, Dement WC.
A predictive morphometric model for obstructive sleep apnea. SDDS
Report. March 1997:8.
3. Guilleminault C, Parinen M, Lollman K, Powell N, Stoohs R.
Familial aggregates in obstructive sleep apnea syndrome. Chest.
1995;107:1545-1551.
4. Kushida C, Guilleminault CA, Mignot E, et al. Genetics and
craniofacial dysmorphism in family studies of obstructive sleep
apnea. Presented at: APSS Conference; June 1996; Washington, DC.
5. Palmer B. Importance of breastfeeding to total health—Section
A, Slides A58-A67 plus all of Section B. Available at: http://www.brianpalmerdds.com.
Accessed December 28, 2002.
6. Mukai S, Mukai C, Asaoka K. Congenital ankyloglossia with deviation
of the epiglottis and larynx: symptoms and respiratory function
in adults. Ann Otol Rhinol Laryngol. 1993;102:620-624. Also available
at: http://www02.so-net.ne.jp/~s-mukai. Accessed December 15,
2002.
7. Price WA. Nutrition and Physical Degeneration. 6th ed. New
Canaan, Conn: Keats Publishing Inc; 1997.
8. Palmer B. The influence of breastfeeding on the development
of the oral cavity: a commentary. J Hum Lact. 1998;14:93-98.
9. Palmer B. The significance of the delivery system during infant
feeding and nurturing. ALCA News. 1996;7:26-29.
10. Palmer B. Importance of breastfeeding to total health, Section
A, Slides A3, A7, A8, & A64. Available at: http://www.brianpalmerdds.com.
Accessed December 28, 2002.
11. Paunio P, Rautava P, Sillanpaa M. The Finnish family competence
study. The effects of living conditions on sucking habits in 3-year-old
Finnish children and association between these habits and dental
occlusion. Acta Odontol Scand. 1991;51:23-29.
12. Melsen B, Stensgaard K, Pedersen J. Sucking habits and their
influences on swallowing pattern and prevalence of malocclusion.
Euro J Orthodont. 1979;1:271-280
13. Davis D, Bell P. Infant feeding practices and occlusal outcomes:
a longitudinal study. J Can Dent Assoc. 1991;57:593-594.
14. Farsi N, Salama F, Pedo C. Sucking habits in Saudi children:
prevalence, contributing factors and effects on the primary dentition.
Pediatr Dent. 1997;19:28-33.
15. Labbok M, Hendershot G. Does breast-feeding protect against
malocclusion? Am J Prev Med. 1987;3:227-232.
16. American Academy of Pediatric Dentistry. Special Issue: Reference
Manual. Pediatr Dent. 1995-1996;17(6).
17. Victora CG, Behague DP, Barros FC, Olinto MT, Weiderpass E.
Pacifier use and short breastfeeding duration: cause, consequence,
or coincidence? Pediatr. 1997;99:445-453.
18. Shepard JWJ, Gefter WB, Guilleminault C, et al. Evaluation
of the upper airway in patients with OSA/SDB. Sleep. 1991;14:361-371.
19. Weider DJ, Sateia MJ, West RP. Nocturnal enuresis in children
with upper airway obstruction. Otolaryngol Head Neck Surg. 1991;105:417-432.
20. Timms DJ. Rapid maxillary expansion in the treatment of nocturnal
enuresis. The Angle Orthodontist. 1990;60:229-233.
21. Zuckerman B, Stevenson J, Bailey V. Sleep problems in early
childhood: continuities, predictive factors, and behavioral correlates.
Pediatrics. 1987;80:664-671.
22. Chervin RD, Dillon JE, Bassetti C, Ganoczy DA, Pituch KJ.
Symptoms of sleep disorders, inattention and hyperactivity in
children. Sleep. 1997;20:1185-1192.
23. Palmer B. Sleep apnea presentation—Section A, Slide
A58. Available at: http://www.brianpalmerdds.com. Accessed December
28, 2002.
24. Palmer B. Importance of breastfeeding to total health—Section
C. Slides C40-C58. Available at: http://www.brianpalmerdds.com.
Accessed December 28, 2002.
25. Merideth GM. Airway and dentofacial development. Am J Rhinol.
1988;2:33-41.
------------------------------------------------------------------------Copyright
© 2004 CurAnt Communications,
an MWC/Allied Healthcare Group Company. All rights reserved.

The Uniqueness of
the Human Airway (Part 1 of 2)
• Prevention
- The Key to Treating OSA/SDB (Part 2 of 2)

 Figure
1. Adult swallowing pattern.
Figure
1. Adult swallowing pattern. Figure
2. Adult tongue-thrust.
Figure
2. Adult tongue-thrust.
